By continuing to use our site, you consent to the processing of cookies, user data (location information, type and version of the OS, the type and version of the browser, the type of device and the resolution of its screen, the source of where the user came from, from which site or for what advertisement, language OS and Browser, which pages are opened and to which buttons the user presses, ip-address) for the purpose of site functioning, retargeting and statistical surveys and reviews. If you do not want your data to be processed, please leave the site.
The Voice of People With Breast Cancer
Education
Our Voices Blog
Tag : breast cancer
Busting Breast Cancer Myths: You Can’t Get Breast Cancer Without a Family History
Having a family history of breast cancer could mean two different things. About 5% to 10% of breast cancer cases are passed down from parent to child. Sometimes, several people in a family may have breast or other types of cancer. But even when no inherited or familial connection is found, breast cancer can still happen unexpectedly.
Busting Breast Cancer Myths: Younger People Don’t Get Breast Cancer
If you are someone under the age of 50, there are a lot of important life events that you can imagine in your future. Getting diagnosed with breast cancer is most likely not on that list of events, and for many young people, especially women, it never will be. However, there has been a growing number of younger women over the past few decades who are developing breast cancer, and researchers are trying to determine why.
Busting Breast Cancer Myths: Men Don’t Get Breast Cancer
When most people think of someone with breast cancer, they think about women. Many are surprised to find out that men can also get breast cancer. Personal stories from patients on websites show how common this myth is, and many men initially express disbelief and shock at being diagnosed with a “woman’s disease”.
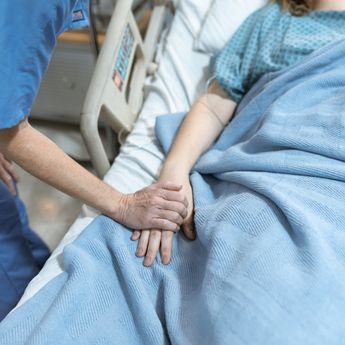
My Breast Cancer Surgery
When I was 15, I ended up in hospital with a ruptured, grapefruit-sized cyst on my left ovary. Two years later, another cyst required a second surgery. Years later, in my early 30s, a perforated appendix landed me back on the operating table. So, when I was diagnosed with breast cancer and surgery became part of my treatment plan, it felt old hat.
Making Sense of Genetic Testing in Breast Cancer - Part 2: What to Expect and How to Access Testing
In Part 1, we looked at what genetic testing is and how it helps us understand breast cancer risk. Now let’s turn to the practical side: what to consider before testing, the possible results, how to get tested, and the role of genetic counsellors.
Players in Healthcare: The Municipal Government
When we think about healthcare, municipal governments might not be the first thing that comes to mind. After all, they don’t run hospitals or provide cancer treatments the way provincial and territorial governments do. But local governments shape the communities where we live, and this has a huge influence on our health and wellbeing.
Making Sense of Genetic Testing in Breast Cancer – Part 1: Understanding the Basics
Genetic testing has become an important tool in understanding breast cancer risk. Whether you’ve heard about BRCA1 and BRCA2 or are just beginning to learn about hereditary cancer, knowing the basics can help you and your family make informed choices. In this first part, we’ll explore what genetic testing is, how it works, and why it matters for breast cancer.
More Than Just a Lump
A lump is one of the most discussed symptoms of breast cancer. However, a lump, and the other well-known signs of breast cancer, are not always the first thing you may notice. You may not even realize what you’re looking at could be a symptom of breast cancer.
Navigating an Intimate Relationship: Avoiding a Communication Breakdown
For most couples, breast cancer is completely new territory, so it’s important for both of you to share how you’re feeling and coping. You can’t expect your partner to automatically understand what you’re going through, and the same goes the other way around. They might not know how to best support you, which is why being open about your emotions, needs, and worries can help you stay connected.
World Breast Cancer Research Day: A Legacy of Compassion for Breast Cancer Care
As we mark World Breast Cancer Research Day on August 18th, we honour the researchers, scientists, and geneticists around the world for their contributions in the advancement of care and research for breast cancer. Here, we focus on some of the people who have made significant differences in improving care.
Players in Healthcare: the Provincial & Territorial Governments
In the second part of our three-part blog series, we are taking a closer look at the role provincial and territorial governments play in healthcare. Spoiler alert, it is a big one!
To Work or Not to Work?
If you are still in the workforce when diagnosed with breast cancer, it is important to understand how it may affect this aspect of your life. Breast cancer is on the rise in women under the age of 50. You may have been diagnosed during a time when you were making meaningful progress in your career or reaching a major professional milestone. It can be a difficult choice to either stop working or continue on throughout your treatment.
Still Burning: Cancer-free but the Heartburn Won’t Quit
Only after being diagnosed with breast cancer and undergoing surgery and treatment did the burning in my throat and chest—the uncomfortable, dry and always-on-fire feeling of heartburn—become a constant in my life. Single-digit years now, cancer-free, I'm still carting a container of Tums in my black Lululemon Everywhere Belt Bag.
Players in Healthcare: The Federal Government
If you’ve ever wondered what role the federal government plays in your healthcare (especially after a breast cancer diagnosis), you’re not alone. Many people may be surprised to learn that while the federal government helps fund healthcare, it doesn’t directly provide hospital or doctor services. Still, it plays several important roles that can affect your treatment and care. Here’s a breakdown of what the federal government does do, how it can matter to you, and some ways you can get involved in advocacy.
Join the TCS Toronto Waterfront Marathon and Fundraise for CBCN
Are you ready to lace up your running shoes for a great cause? On October 18 and 19, 2025, thousands of participants will hit the streets for the TCS Toronto Waterfront Marathon, and this year, you can make every step count by fundraising for the Canadian Breast Cancer Network (CBCN)!
Familial vs Hereditary Breast Cancer: What’s the Difference?
About 5% to 10% of breast cancer cases are passed down through families. Sometimes, several people in a family may have breast or other types of cancer, even if no specific gene mutation is found. This is called familial breast cancer. Having a family history can raise your risk, but it doesn’t always mean the cancer is genetic.
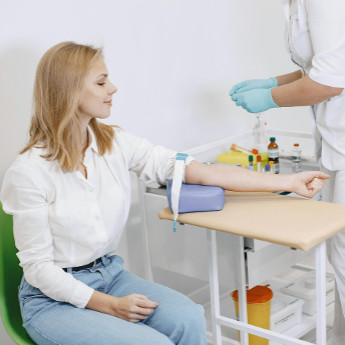
The Emerging Roles of Circulating Tumour DNA and Liquid Biopsies
When going through breast cancer, you often hear about different kinds of tests like scans, biopsies, and blood work. One new kind of test that’s starting to gain attention uses ctDNA or circulating tumour DNA. You may also hear it called a liquid biopsy. But what is it? And how could it help in breast cancer care?
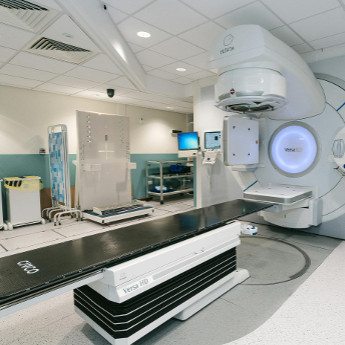
Radiation 411
Radiation therapy: two words that sounded surreal when I heard them attached to my cancer treatment plan. I knew what radiation was, technically, but I was clueless about what the actual experience would be like or how it would affect me. Mostly because my oncology team had described it and its potential side effects in vague terms. Apparently, this isn’t unusual for women like me who’ve been diagnosed with breast cancer.
Dancing Through Diagnosis, part 2
There was a total of three oncologists from different areas of care that I would meet along the way. Then there is my plastic surgeon! The beginnings of a joke. Three oncologists and a plastic surgeon go into a bar... If you have a good joke for this scenario, I would love to hear it. But this is the thought that keeps popping into my head every time I am told about my surgical team.
Dancing Through Diagnosis, part 1
As my towel brushed past the bottom of my right breast, I couldn’t help noticing that something didn’t feel right. Broken glass? It felt like broken glass. Is that possible? Could I have broken my boob? Can you break a boob? My mind began to swirl toward real questions then to ones that were clearly insane and made no sense... and yet, I asked them out loud... to myself... in the mirror.