By continuing to use our site, you consent to the processing of cookies, user data (location information, type and version of the OS, the type and version of the browser, the type of device and the resolution of its screen, the source of where the user came from, from which site or for what advertisement, language OS and Browser, which pages are opened and to which buttons the user presses, ip-address) for the purpose of site functioning, retargeting and statistical surveys and reviews. If you do not want your data to be processed, please leave the site.
The Voice of People With Breast Cancer
Education
Our Voices Blog
Tag : treatment
Ageism and the Treatment of Breast Cancer
A Power Point presentation titled “Ageism and Health” from the Waterloo-Wellington Older Adult Council crossed my desk recently and caused me to reflect on my own experience of breast cancer diagnosis and treatment. I was diagnosed in 2024 when, at the age of 74, a routine mammogram identified an anomaly in my left breast. So started the long process of referrals, tests, diagnosis and treatment.
The Messy, Honest Truth About Diagnosis, Recovery and the Emotions No One Talks About
I’m an open book about breast cancer. I’ve chosen to be vocal because I want to wipe out stigma, shine light on little-talked about topics and help other women feel less alone. When I was first diagnosed with breast cancer, it didn’t cross my mind that one day I’d want to share all the details about my personal experiences with cancer by writing a monthly column, but life is weird and here I am. And I’m grateful. Especially when I receive a direct message on my Instagram from a woman I don’t know, who is dealing with her own breast cancer diagnosis and looking for support.
Still Burning: Cancer-free but the Heartburn Won’t Quit
Only after being diagnosed with breast cancer and undergoing surgery and treatment did the burning in my throat and chest—the uncomfortable, dry and always-on-fire feeling of heartburn—become a constant in my life. Single-digit years now, cancer-free, I'm still carting a container of Tums in my black Lululemon Everywhere Belt Bag.
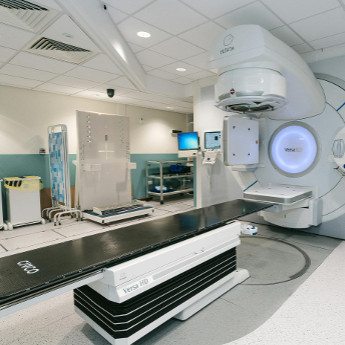
Radiation 411
Radiation therapy: two words that sounded surreal when I heard them attached to my cancer treatment plan. I knew what radiation was, technically, but I was clueless about what the actual experience would be like or how it would affect me. Mostly because my oncology team had described it and its potential side effects in vague terms. Apparently, this isn’t unusual for women like me who’ve been diagnosed with breast cancer.
Why Clinical Trials Are Crucial for People with Breast Cancer
Breast cancer remains one of the most common cancers worldwide. While progress in early detection and treatment has significantly improved survival rates over the past few decades, continued advancement depends on clinical trials. These research studies are the foundation of medical progress, playing a vital role in finding better ways to prevent, diagnose, and treat breast cancer.
What I’ve Learned About Breast Cancer Vaccines
Breast cancer vaccines are a buzzy topic that’s seemingly everywhere lately—from ongoing news stories about cancer research to Reddit threads and personalized Instagram posts. But what I’m most interested in knowing is if these vaccines are truly the “golden goose” every woman like me, who is dealing with a breast cancer diagnosis or the aftermath of one, is looking for: can these vaccines truly alleviate my fear by ensuring zero recurrences? To find out, I did a deep dive into the latest information and here’s what I learned.
Can You Do the Tamoxifen Time?
I’m a Tamoxifen fail. I quit taking the drug just shy of my five-year prescription’s halfway mark. The estrogen-blocking pill fried my short-term memory within the first 14 days and then, tormented me daily with its version of Jay-Z’s “99 Problems.” And lucky me. I experienced every single one of them.
We Asked You About Chemotherapy Side Effects
Experiencing side effects from breast cancer treatment is a common occurrence for patients. While systemic chemotherapy, radiation, and targeted therapy are effective treatments for breast cancer, learning to cope and live with their unwanted or unexpected side effects can be challenging. We reached out to breast cancer patients to hear about their experiences with this.
Humour in Times of Crisis pt. 2 - Excerpts from Angel in the Marble
The minute you get a cancer diagnosis, you start looking for the magic cure. For me, this meant researching the hell out of the disease and revamping my lifestyle, exercise regime, spiritual practice, and diet. Within days, I knew the latest cancer breakthroughs and snake oil salesman’s remedy for the problem. And I took on the task of miraculous cure (and possible canonization) with a vengeance. Turmeric was the new gold standard. I popped four pills a day and drank Indian golden milk and turmeric lemon tea morning, noon, and night. My skin oozed Trumpian orange, my countertops glowed with permanent yellow stains, and man, did I feel good. I knocked back shots of apple cider vinegar chased by pomegranate juice. I downed hemp hearts, chia, flax, and bee pollen. My daughter Sonja arrived one day with the Holy Grail—a Vitamix— and it became my cauldron, a sacred vessel for preparing healing concoctions laced with kale, ginger, blueberries, and coconut water.
Your Questions Answered About Disputing Denied Insurance Claims Through the OmbudService for Life and Health Insurance (OLHI)
A common inquiry we receive from patients is what to do if their insurance company has denied their claim related to their cancer treatments. One service we often direct individuals to is the OmbudService for Life and Health Insurance (OLHI). But who are they? And how can they help you?
Getting a Second Opinion in our Public Health System
When we hear stories about people’s experiences receiving a diagnosis like breast cancer, we often hear the empowering message to trust your gut and get a second opinion if the answers aren’t sitting well with you. These messages, while meant to be inspiring, can often feel impractical. In other countries, like the US, getting second opinions may be fairly straightforward, but in Canada, second opinions may be a bit trickier to come by.
How Race and Ethnicity Can Influence Breast Cancer
According to the World Health Organization (WHO), breast cancer is the most common form of cancer, with more than 2.2 million cases in 2020. It is estimated that 1 in 12 women will develop breast cancer and it will be the primary cause of death among all other types of cancer in women. However, breast cancer survival has improved significantly since the 1980s due to increased early detection, screening programs, and improved treatment options.
Three Things to Know Before Your Lumpectomy
I’m a talker. I like to communicate and sometimes, okay often, I’m an over-sharer. I need to know what’s going on and why and in my version of yin and yang, I believe that because I’m an open book everyone else will be too. Except, not so much.
Estro-Belly
I have been struggling with my body image these last 8 weeks. The funny thing is that it’s not with the two scars I have running across my chest. I have actually adapted well to that change, even with my right scar being lumpy and misshapen. What I have been struggling with is my weight gain thanks to Tamoxifen. Without estrogen, my mid-section is taking on the appearance of a barrel. A barrel made of pudding, with an oatmeal crust! Having always been fit and healthy, I am finding myself disturbed by this body morphing of mine.
I Had to Work During Cancer Treatment and it Sucked
I worked during my entire breast cancer treatment. I didn’t want to. I had to. I live alone. I don’t have a husband or boyfriend. I pay my bills on time and by myself. Yes, it was a choice, but it was a horrible one.
Coping With Scanxiety
Scanxiety may not officially be a real word, but the feelings it brings about are real. Very Well Health defines scanxiety as the term used to “describe the anxiety people with cancer feel while waiting for scans”. Regardless of whether the scans are for diagnostic purposes, monitoring treatment, checking recurrence or as a check-up, individuals can experience apprehension before, during, and while waiting for the results of their scans. The apprehension and fear that is felt can range from feeling claustrophobic in the scan machine to imagining the worst-case scenario of the scan results. Many people experience scanxiety so it is important to learn coping techniques that help eliminate the anxiety.
Have Hair, Do Care
Breast cancer made my hair thicker. And wavy-er. Not right away obviously. It’s not like it was a special prize I was gifted with to make up for the shock and fear of being diagnosed with breast cancer.
Tamoxifen. It’s Saving My Life, But it’s Killing My Self-esteem
I could cry writing this. Or maybe screaming for five minutes into a pillow so my neighbours don’t hear me would feel better. The walls in my condo aren’t that thick. Either way, my reality’s not changing any time soon. And by reality, I mean my body and the extra weight it has been lugging around since I started taking Tamoxifen a year ago.
Clinical Trials Part 2: Debunking Common Myths About Clinical Trials
In part 1 of our blog series on clinical trials, we explained what clinical trials are, why you should participate in them and how to get more information about participating. You may now be familiar with clinical trials but still hesitant about enrolling in one because of certain concerns that you may have. These concerns are valid as many breast cancer patients have these same concerns. However, some of these concerns about clinical trials are ill-informed. In part 2 of our blog series on clinical trials, we debunk some of the most common myths surrounding clinical trials. We hope that this will provide you with some fact-based information to make a more informed decision about whether or not clinical trials are right for you.
Clinical Trials Series Part 1: What Are Clinical Trials and Are They Right for Me?
According to a 2014 study by the Canadian Partnership Against Cancer, less than 7% of adult cancer patients enrolled in clinical trials.1 This may be because many cancer patients are not aware of clinical trials, do not know how to enroll in them or are concerned that they are unsafe. In part one of our blog series on clinical trials, we explain what clinical trials are to provide you with the right tools to decide whether you should enroll in a clinical trial.