By continuing to use our site, you consent to the processing of cookies, user data (location information, type and version of the OS, the type and version of the browser, the type of device and the resolution of its screen, the source of where the user came from, from which site or for what advertisement, language OS and Browser, which pages are opened and to which buttons the user presses, ip-address) for the purpose of site functioning, retargeting and statistical surveys and reviews. If you do not want your data to be processed, please leave the site.
The Voice of People With Breast Cancer
Education
Our Voices Blog
Tag : metastatic breast cancer
Ringworm: Tamoxifen’s Secret Side Effect
Trapped beneath my bra, cotton t-shirt and cropped pants, pools of sweat mingled with dust and grime before being absorbed into my clothes and skin. Despite the cold showers I soaped up under twice daily, one before heading out into the wee hours of the morning and another again in the dark of night before crawling under a thin sheet to sleep, the dirty damage was done. A skin fungus had formed. I had ringworm.
Taking the Plunge: Breast Cancer and the Dating Pool
The thought of dating after a breast cancer diagnosis and treatment might make you nervous or excited. It may also reawaken or increase emotional responses you had at diagnosis or during treatment. If you have anxiety or depression, these responses can cause you to focus on or magnify negative thoughts about your prospects for dating. If you want to date but feel reluctant to start, you might be having difficulty imagining yourself meeting new people and having fun.
FinNav Five: Government Programs
The negative financial impacts after a breast cancer diagnosis can be strenuous, especially for those already in a precarious financial situation prior to being diagnosed. Already having to deal with the overwhelming feeling of being diagnosed with breast cancer, patients should be able to focus on their health and not have the added stress of dealing with their financial situation. That is why we created FinancialNavigator, an online database of various financial assistance programs across Canada.
Highlights from ASCO 2023
The 2023 American Society of Clinical Oncology (ASCO) annual meeting was held from June 2 to 6. CBCN was pleased to be able to attend and participate in the many interesting and groundbreaking research that was shared at ASCO this year. Below, we present a few highlights and takeaways from this year’s conference.
Show Me the Money. Five Ways You Can Receive Financial Support
When I was diagnosed with breast cancer, I had no idea how hard it would be. Not the surgery, I’ve had major surgery before, so I wasn’t afraid of being put under anesthetic and being operated on. Mentally, I was focused on one sole factor, survival, so my head space at the time was very clear and didn’t allow for any other emotions or thoughts. Reality, fear, anxiety, hope…that all came later.
Addressing the Healthcare Needs of Indigenous Populations
June 21, 2023 is National Indigenous Peoples Day. This is a day for all Canadians to recognize and celebrate the unique heritage, diverse cultures and contributions of First Nations, Inuit, and Métis peoples. This is also a day that should call to attention the various issues that Indigenous peoples continue to face, including racism, colonialism, and disparate health outcomes from much of the rest of Canada. Broad determinates of health like geography, accessibility and availability of services, and cultural differences contribute to the challenges faced by Indigenous peoples.
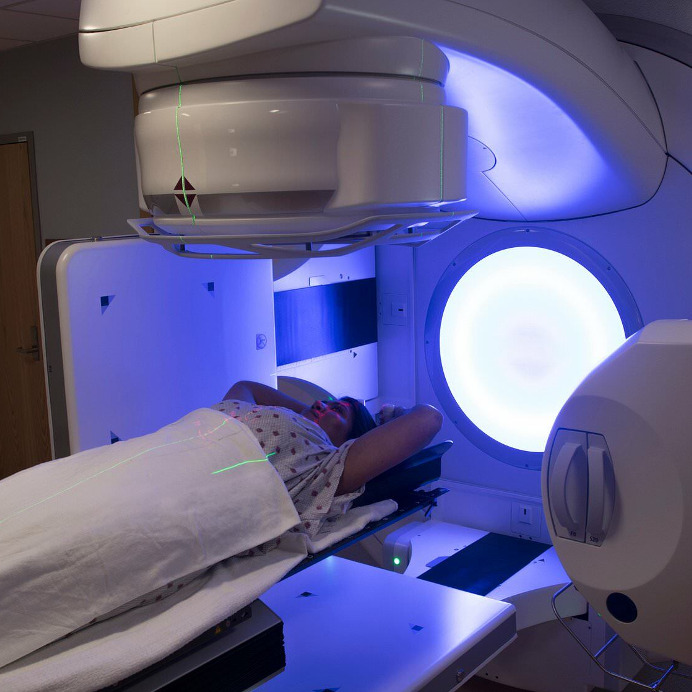
Reason #5 Cancer Still Sucks: Radiation Therapy is Hit or Miss
The fifth reason that cancer still sucks is that although radiation therapy can be an effective cancer treatment, it may fail to kill some of the tumor cells in its path, or it may miss some tumor cells completely. In addition, while “palliative” radiotherapy can dramatically improve symptoms in some individuals with incurable cancers, it may have minimal impact or provide only very brief relief to others.
“Mommy Has Cancer”: The Most Difficult Conversation to Have
In February 2019, five days after my birthday, I found a tiny, split pea lump in my right breast. I immediately went to my GP, who sent me for a mammogram and ultrasound. The first available appointment was the following week. The mammogram went “squishingly” and then I was shuffled off for my ultrasound. Afterwards, the technician told me they needed to review the images with the radiologist to make sure they had everything they needed. I didn’t really think twice about it as that seemed to be the normal practice during my pregnancy.
I Am a Mother with Cancer
I am a metastatic breast cancer patient with liver and spine metastases. I am also a mom and a grandmother. One day, I felt a very hard pea-sized lump right under the skin. My family physician sent me for a mammogram and ultrasound. The radiologist came in and said he was concerned and brought me back the following day for a biopsy. I was diagnosed with invasive ductal carcinoma. I was petrified and scared. Since working at a cancer centre, I had every bad scenario going through my mind. I had a double mastectomy followed by four months of chemotherapy and seven weeks of radiation. It was difficult losing my hair, feeling nauseous and weak but I was determined to beat this horrible disease.
We Asked You About Chemotherapy Side Effects
Experiencing side effects from breast cancer treatment is a common occurrence for patients. While systemic chemotherapy, radiation, and targeted therapy are effective treatments for breast cancer, learning to cope and live with their unwanted or unexpected side effects can be challenging. We reached out to breast cancer patients to hear about their experiences with this.
I Don’t Look Sick: My Life with MBC
I have advanced stage 4 Metastatic Breast Cancer (MBC). MBC is when breast cancer has spread to other parts of the body. Typically, it spreads to the bones, liver, lungs, and brain. There is currently no cure for MBC but there is treatment, and some women can live for many years.
I Only Wanted One Surgery, So I Chose AFC Reconstruction
This year 28,000 women in Canada will be diagnosed with breast cancer. On March 10, 2022, I became one of those women. Disturbingly, within a month of my diagnosis, two more of my close friends received their breast cancer diagnoses. In total, I have 15 close friends and counting who are either breast cancer survivors, or who are currently battling breast cancer. This silent epidemic seems to be growing at an extraordinary pace.
Highlights From the 2022 San Antonio Breast Cancer Symposium (SABCS)
The San Antonio Breast Cancer Symposium (SABCS) is the annual breast cancer conference that brings together researchers, clinicians, patients and manufacturers from all over the world to discuss the latest breast cancer research. Last December, we were pleased to be able to attend in-person, and we'd like to share with you the highlights from SABCS.
Our Top Blog Posts for 2022
The past year allowed us a return to a more normal routine in a lot of ways, and our blogs from 2022 reflect that. Posts about being able to gather for the holidays, get mastectomy tattoos, and having in-person healthcare visits were some of the topics of our top 10 blog posts from last year.
2022: Our Year in Review
CBCN connects patients, caregivers, health care professionals, researchers, public health agencies and industry stakeholders to improve knowledge translation and promote optimal health outcomes for Canadians with breast cancer. We do this through the promotion of information sharing, education, and advocacy activities. As we look forward to the new year, we would also like to look back on 2022 and share what CBCN has achieved on behalf of Canadian breast cancer patients, their loved ones, and caregivers.
FinNav Five: Experiences, Services, And Travel Assistance
Depending on your situation, your financial needs can come in different forms, from needing money to pay for rent, to needing help with paying for treatments, to requiring help with parking costs when you go for cancer treatments. To highlight the various types of programs listed in FinancialNavigator, we have put together this blogpost series.
We Are Not Counted
I am writing this from my hospital bed. One of many cancer-related hospital stays and visits. This hospital has become my second home. Fortunately, it’s a great hospital. That doesn’t mean I want to spend a lot of time here though. But that is inevitable when you have metastatic breast cancer, otherwise known as mBC. That is Stage IV cancer. Cancer that has travelled outside the breast and has metastasized into other areas of the body.
I Can Create My Reality
I read a lot. About everything, really, including Jackie Collins’ Hollywood Wives, which I’m about three decades late on, I know, but I just watched Lady Boss, The Jackie Collins Story on Netflix so here I am. The book is good too, in a dishy fantastical way, so naturally after 15 pages in I went back online and bought the sequel Hollywood Wives: The New Generation. But, that’s not the kind of reading I want to share. Books about the power of the mind, self-esteem, and mental health and how to create a positive reality are what I’m referring to. I like these types of books and have piles of them, because I honestly believe they work. I just wish I’d fallen back on them when I was initially diagnosed with breast cancer and going through surgery and treatment.
History of the BRCA 1 & 2 Genes
Before it was known that genes could be linked to various cancers, 1970s research focused largely on viruses and their role in the development of cancer. With the knowledge that family history had an impact on cancer risk, Mary-Claire King, an American geneticist, began to theorize possibilities beyond viruses and started her mission in identifying the cause of breast cancer running in families.
Breast Cancer Care for Lesbian and Bisexual Women
Who you are and where you live can greatly impact your access to care, and sexual orientation is no exception to this. Within the healthcare system, the LGBTQ+ community regularly experiences barriers when seeking adequate health services, and the effect of these barriers may result in poorer health outcomes. This leads to the question — does being a lesbian or bisexual woman affect your risk for breast cancer?