By continuing to use our site, you consent to the processing of cookies, user data (location information, type and version of the OS, the type and version of the browser, the type of device and the resolution of its screen, the source of where the user came from, from which site or for what advertisement, language OS and Browser, which pages are opened and to which buttons the user presses, ip-address) for the purpose of site functioning, retargeting and statistical surveys and reviews. If you do not want your data to be processed, please leave the site.
The Voice of People With Breast Cancer
Education
Our Voices Blog
Tag : young women
In Between Moments
In May 2025, at the age of 40, everything changed for me. I was diagnosed with breast cancer. My journey through cancer lasted 10 months, three surgeries, chemotherapy, and now 5 to 10 years on an estrogen blocker that has put me into early menopause.
What We Don’t Know (and it’s a lot), Should Know, About Canada’s Breast Cancer Screening Guidelines
How old were you when you first learned you were eligible for a mammogram? If you’re like me, that information only became clear after you found a lump of your own. And at that point, the rules and guidelines about when women can and can’t access breast cancer screening don’t feel relevant anymore—it’s too late. Except that it shouldn’t be.
From Diagnosis to “I Do”: Finding Life After Breast Cancer
I was just 27 years old, newly engaged and planning my wedding, when I was diagnosed with HER2+ Stage 2 breast cancer. Overnight, my world shifted from picking out flowers and venues to chemotherapy appointments, surgery dates, and a treatment plan that included chemo, surgery, and radiation.
Busting Breast Cancer Myths: Younger People Don’t Get Breast Cancer
If you are someone under the age of 50, there are a lot of important life events that you can imagine in your future. Getting diagnosed with breast cancer is most likely not on that list of events, and for many young people, especially women, it never will be. However, there has been a growing number of younger women over the past few decades who are developing breast cancer, and researchers are trying to determine why.
To Work or Not to Work?
If you are still in the workforce when diagnosed with breast cancer, it is important to understand how it may affect this aspect of your life. Breast cancer is on the rise in women under the age of 50. You may have been diagnosed during a time when you were making meaningful progress in your career or reaching a major professional milestone. It can be a difficult choice to either stop working or continue on throughout your treatment.
Dancing Through Diagnosis, part 1
As my towel brushed past the bottom of my right breast, I couldn’t help noticing that something didn’t feel right. Broken glass? It felt like broken glass. Is that possible? Could I have broken my boob? Can you break a boob? My mind began to swirl toward real questions then to ones that were clearly insane and made no sense... and yet, I asked them out loud... to myself... in the mirror.
We All Have A Purpose
In December 2016, I was diagnosed with Stage III HER2-positive Invasive Ductal Carcinoma, two months after my 39th birthday. It was one of the scariest times of my life. It felt unreal at first and everything became a haze instantly. I never imagined I would hear those words and that they would be talking about me. The next thing I remember is the doctor telling me that they know exactly what to do, and that the survival rate was 88% and I should focus on that. To be honest, most of what she said that day sounded to me like jumbled up words. I allowed myself to cry on the day I was diagnosed but very early on, I decided to only focus on what life would be after cancer.
Younger Women and Breast Cancer Care Equity
The spending justifications for girl math are funny. But they just aren’t real. And oddly, this type of rationalization reminds me of how many doctors dismiss younger women when they believe that they have breast cancer. I know this because it happened to me. This is how I see girl math being applied to breast cancer.
My Genetic Test Results Changed my Treatment Plans
Stacy Zelazny lives in a tiny town in Ontario, literally, she resides in a little-known place called Tiny, Ontario. Stacy describes herself as a mom of two amazing girls who is married to her best friend and winning the biggest fight of her life.
Being Diagnosed with Breast Cancer During a Pandemic
My name is Katharina and I was diagnosed with stage 2a breast cancer in March 2020 just when the pandemic was starting. I was 25 years old at the time. I had to go through testing and treatment alone without any support person by my side.
The innocence of a toddler and the reality of cancer
It was just another typical morning in our house, trying to get my son fed and dressed before I take him to daycare. As I am multitasking, getting myself dressed and making sure my son is actually brushing his teeth, I notice he’s watching me. He’s still trying to process those two large scars across my chest. The incisions are still fresh and slowly healing and turning to scars. Scars that represent where my breasts once were but now is just an empty space. He finally pipes up. “When are your boobies going to grow back, Mommy?” He asks so innocently.
What’s important for patients to know from the 2017 San Antonio Breast Cancer Symposium?
Every year clinicians, researchers, patient advocates and industry members head to Texas to share the latest breakthroughs in breast cancer research. It’s a key conference to learn about new treatments or new standards of care for breast cancer patients. Here’s some of the highlights that have the most impact on patient care today:
My metastatic breast cancer has disappeared
On July 19, 2011, at the age of 33, I was diagnosed with breast cancer. With a 10-month-old son, I was still glowing with the joy of motherhood—but when a lump that I had been attributing to breastfeeding challenges refused to go away, I decided to see my doctor.
Personalized medicine: A revolution in cancer treatment
The more researchers and doctors learn about cancer, the more they are beginning to understand that there isn’t one standard approach to treating it but many factors to consider to come up with the best treatment plan for each person. New research is adding to this knowledge and instead of treating a cancer based on its location in the body, clinicians are starting to personalize and improve treatments for individual patients based on genomics.
Facing triple positive breast cancer
My life changed forever once I received the phone call no one wants to get early one morning in March 2015. My surgeon was on the other line with the results from my recent biopsy. The lump that was supposed to be only a pesky cyst was indeed cancerous. The surgeon further explained my diagnosis. But the only thing I heard was that I had cancer. My world felt like it was spinning out of control.
What More Looks Like …
Looking back at the 4 years we have hosted our event, the Pink Ribbon Project (PRP) is always interesting, emotional and clarifying. We can see the things we have accomplished and learned but most importantly where we can grow in our work around breast cancer.
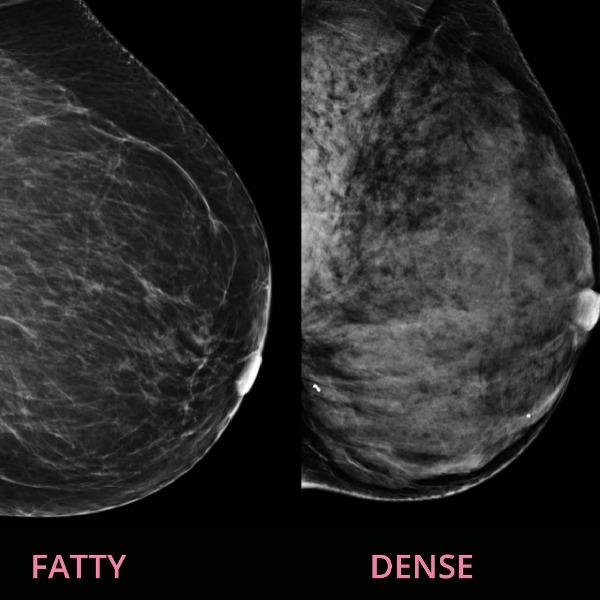
What is Breast Density and Why Does It Matter?
Roughly 40% of Canadian women, meaning about 3 million women, have what is known as “dense breasts.” Dense breasts are normal and common, but they also pose cancer risks and screening challenges. Breast density can have a significant impact on cancer detection and the treatment and prognosis of a diagnosed cancer. Many women in Canada are unaware of their breast density, impacting their screening and their ability to be their own breast health advocate. Why is knowing and understanding your breast density so important?
You Can’t Fix Breast Cancer But You Can Make it Better
On November 3, 2011, I received a phone call while waiting in line to pick up my sons, 2 and 4, from school. On the other end of the line was my wife’s GP advising me that Kate had a rare and aggressive form of breast cancer. The ensuing months brought bewilderment, fear and anger. I struggled to find a way to express what was happening to our family and to provide care.
Olive Us Care provides childcare for families facing cancer
If you or your child has a cancer diagnosis and you need childcare in the Greater Hamilton Area of Ontario, Olive Us Care can help.
This new non-profit can provide up to 10 hours per month of free in-home childcare for children under 12 years of age.
Young mother faces metastatic breast cancer
In 2014, Krista Dumas of Kirkland Lake, Ontario, was shocked to receive a diagnosis of metastatic breast cancer at the age of 33. The cancer was in her liver and L5 vertebrae.












.jpeg)