By continuing to use our site, you consent to the processing of cookies, user data (location information, type and version of the OS, the type and version of the browser, the type of device and the resolution of its screen, the source of where the user came from, from which site or for what advertisement, language OS and Browser, which pages are opened and to which buttons the user presses, ip-address) for the purpose of site functioning, retargeting and statistical surveys and reviews. If you do not want your data to be processed, please leave the site.
The Voice of People With Breast Cancer
Education
Our Voices Blog
Tag : metastatic breast cancer
Genetic Counselling Q&A
A genetic counsellor is a health care professional with specialized education, training, and experience in medical genetics and counselling. Genetic counsellors work with both individuals and families that have a medical, family history, or potential risk for an inherited condition. The role of a genetic counsellor is to identify families at risk for genetic conditions, provide information and supportive counselling, coordinate and review testing options, and connect patients/families with appropriate community resources.
Bringing Awareness and Motivation to Exercise
It is a well-known fact that exercise has been proven to help with cancer-related fatigue, helping to manage the weakness and pain experienced due to treatment and its side effects, as well as de-conditioning. When you’re in pain, tired and feeling ill, it can be challenging to find the motivation to prioritize activity, but several studies show that performing a combination of strength, aerobic and flexibility exercise can help curb the symptoms that hold back our quality of life.
Laboratory Blood Tests, Why So Many?
Throughout the course of a medical diagnosis, members of your health care team will order different laboratory blood tests. Many times, these laboratory blood tests will be repeated throughout the diagnosis, treatment, follow-up, and continuing care. Each medical diagnosis and treatment has specific factors that are required to be monitored. When it comes to the results of these tests and what counts are normal or not, it is important to know that “normal” ranges simply reflect average values in a population. It is common for some tests to be slightly outside of the “normal range” (low or high) without consequence and your clinicians can guide you with respect to their relevance.
Three Things to Consider if You’re Thinking About Going Off Tamoxifen
Chances are, if you have breast cancer you’ve heard about Tamoxifen. I remember the first time my oncologist talked to me about the chemo-infused hormonal-therapy drug. It was during my weekly check-up when I was still having daily radiation. He explained that because the cancer cells found in my right breast were 95 per cent estrogen and progesterone receptor positive, my body’s natural hormones could attach to the cancer cells and help them grow. Obviously I didn’t want that, so I said yes to the drug without even hesitating.
How Race and Ethnicity Can Influence Breast Cancer
According to the World Health Organization (WHO), breast cancer is the most common form of cancer, with more than 2.2 million cases in 2020. It is estimated that 1 in 12 women will develop breast cancer and it will be the primary cause of death among all other types of cancer in women. However, breast cancer survival has improved significantly since the 1980s due to increased early detection, screening programs, and improved treatment options.
Self-Advocacy Tips: For Patients, From Patients
Last year, we wrote a blogpost on the importance of advocating for yourself as someone with breast cancer. We also shared tips on how to go about becoming an advocate and being a part of your healthcare team. While the information shared is valuable and reflects situations you may find yourself in, we believe that the best way to learn is to hear from people who have been there already.
Patient Advocacy with Integrity
Increasingly, the not-for-profit advocacy world has been questioned regarding industry funding. Many critics believe that any organization that receives funding from the pharmaceutical industry is automatically biased, but this ignores the great pains that health charities often go through to remain unbiased, ethical, and credible. And it certainly does not reflect the patient-centric approach that CBCN takes.
Living with Breast Cancer: Living Positively, Exercising Safely
Living through breast cancer is a challenging journey. You will be searching for answers and information about the disease and its treatment; trying to understand how to live positively, and simply reckoning with what your future may look like.
Preventative Treatment for Hereditary Breast Cancer
If you are at high risk for developing breast cancer because of family history or because you have the BRCA1 or BRCA2 gene mutation, you have several preventative treatments to consider. These options include close surveillance, chemoprevention, and prophylactic mastectomy, with or without breast reconstruction.
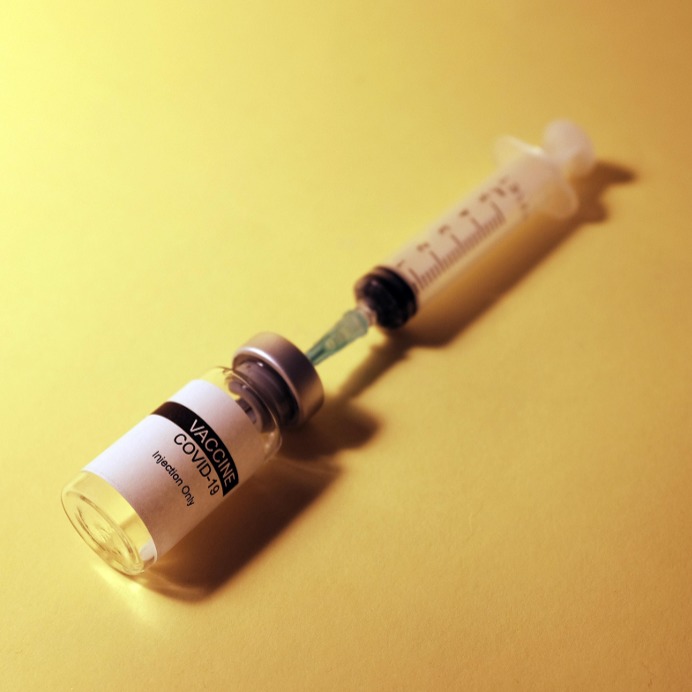
Oncologists Share What You Should Know About the COVID-19 Vaccines
When the COVID-19 pandemic was first declared in March 2019, there was a lack of information about the virus. As time went on and more and more research was conducted, we were able to learn more about how the virus worked, who it was infecting, its symptoms and more. One of the pieces of information from this research was that cancer patients were more likely to have adverse outcomes if diagnosed. Although there was not enough evidence to pinpoint which cancers made individuals more susceptible or enough research to definitively say whether past and present patients had the same concerns, the few findings were enough to label individuals diagnosed with cancer as high-risk. Of course, one’s risk level is dependent on many different factors and varies from person to person.
World Lymphedema Day 2021: Making Treatment More Accessible
The goal of World Lymphedema Day is to make cures for lymphedema and lymphatic diseases a global priority. It is an annual awareness event with participation in many countries around the world. The Lymphedema Association of Ontario (LAO) has committed to improving the lives of people living with lymphedema since it began in 1996 and has become a more dynamic organization in the last year. World Lymphedema Day offers us an opportunity to continue our advocacy and awareness work. LAO partners with hospitals, our professional members, and patients to bring attention to lymphedema in Ontario.
Parenting in the Midst of Trauma
My oldest son is 17. Then 14, and 10- and 6-year-old twins. While I don’t claim to be any kind of parenting expert, I’ve had enough experience now to know a thing or two.
This World Cancer Day, Commit to Act
February 4th is recognized as World Cancer Day, a global initiative led by the Union for International Cancer Control (UICC) that is focused on awareness, education and action. The goal of this day is to create a world where death from cancer is preventable and where everyone can access proper care and life-saving treatment.
Research Highlights from the 2020 San Antonio Breast Cancer Symposium
The San Antonio Breast Cancer Symposium is the annual breast cancer conference that brings together researchers, clinicians, patients and manufacturers from all over the world to discuss the latest breast cancer research. While the 2020 symposium was held virtually, there was still an incredible amount of new research shared.
Will Pharmacare Finally Be a Reality in Canada?
While Canada has a universal healthcare system, this system does not universally cover prescription drugs, nor does it address out-pocket-costs that many, including breast cancer patients, face when they navigate our healthcare system. Every country that has a universal healthcare system also has universal prescription drug coverage – every country but Canada. This results in unequal access to treatment based on a variety of factors, such as where a person lives, the type of insurance they have, their age, their income, and more. To address this, many have suggested implementing national pharmacare – a universal drug coverage system that is publicly funded. We’ve written on pharmacare in the past, on what it is and why it should matter to breast cancer patients and on where Canada’s federal parties stand on pharmacare.
Our Top Blogs From 2020!
2020 was eventful, to say the least. It was a year where many had to shift and pivot from their everyday normal. Appointments were cancelled, surgeries were delayed and rescheduled, and patients found themselves having to access their doctors and healthcare team through a screen. Breast cancer patients had to not only worry about their risk of contracting the COVID-19 virus, but they also had to maintain their cancer care as best they could, something that was a challenge both mentally and physically.
CBCN In Action in 2020: Our Year in Review
As the year slowly winds down, we look back on some of the many activities and projects that CBCN has participated in, developed, or updated. These efforts reflect our ongoing commitment to that ensure that the voice and perspectives of breast cancer patients are reflected in the work that we do.
Why It’s Important to Be Your Own Advocate
The Merriam-Webster dictionary defines ‘advocate’ as a verb that means “to support or argue for”. ‘Self-advocacy is defined as “the action of representing oneself or one's views or interests”. While the word, advocate might make us think of protests or political signs, that is not always the case. As someone with a breast cancer diagnosis, self-advocacy and being an advocate simply means being a part of your health care team. It means knowing yourself and speaking up for yourself to make sure that your cancer care needs are met. Self-advocacy is part of participatory medicine where “patients are actively working alongside their physicians to choose the best course of cancer treatment.”
Metastatic Breast Cancer: The Latest Research and Clinical Trials
Research on breast cancer, and more specifically, metastatic breast cancer (mBC), is critical in helping us better understand this disease. While widespread knowledge of mBC is still limited, there are studies that look specifically at the detection, prognosis and treatment of this type of breast cancer. Similarly, clinical trials on metastatic breast cancer are crucial in helping researchers improve the current standard of care. Below are some of the latest research and some currently recruiting clinical trials on metastatic breast cancer.
Talking Palliative Care Part 6: Funeral Planning: How this dreaded task may actually provide some relief
Planning a funeral, especially if it’s your own, might be one of the most painful and challenging tasks that any of us will have to complete. The very idea can be overwhelming, anxiety causing and heartbreaking to even think about. That being said, so many people share that while they dreaded the idea of having to plan their own funeral, they often experienced a tremendous sense of peace and the feeling of having a huge weight lifted off their shoulders after completing this process. Since the period after the death of a loved one is incredibly distressing to families, pre-planning a funeral can relieve them of some of the stress and can also give you peace of mind that your wishes are being carried out.