By continuing to use our site, you consent to the processing of cookies, user data (location information, type and version of the OS, the type and version of the browser, the type of device and the resolution of its screen, the source of where the user came from, from which site or for what advertisement, language OS and Browser, which pages are opened and to which buttons the user presses, ip-address) for the purpose of site functioning, retargeting and statistical surveys and reviews. If you do not want your data to be processed, please leave the site.
The Voice of People With Breast Cancer
Education
Our Voices Blog
Tag : cancer treatment
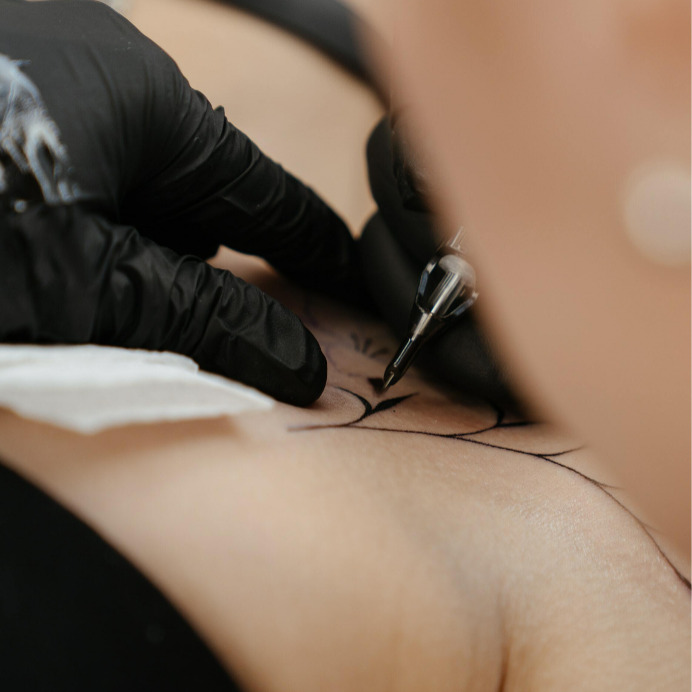
Considering a Mastectomy Tattoo? Here’s What You Need to Know
Following breast cancer surgery, there are a variety of options available to you. You may choose to live flat, have breast reconstruction, get implants, or use breast prostheses. Another option that you may have not considered or known about are mastectomy tattoos. Women who have gotten mastectomy tattoos following their breast cancer treatment have given a variety of reasons for getting them, including that they are a confidence boost following treatment, to cover scars, to create something beautiful, and to mark what they’ve been through.
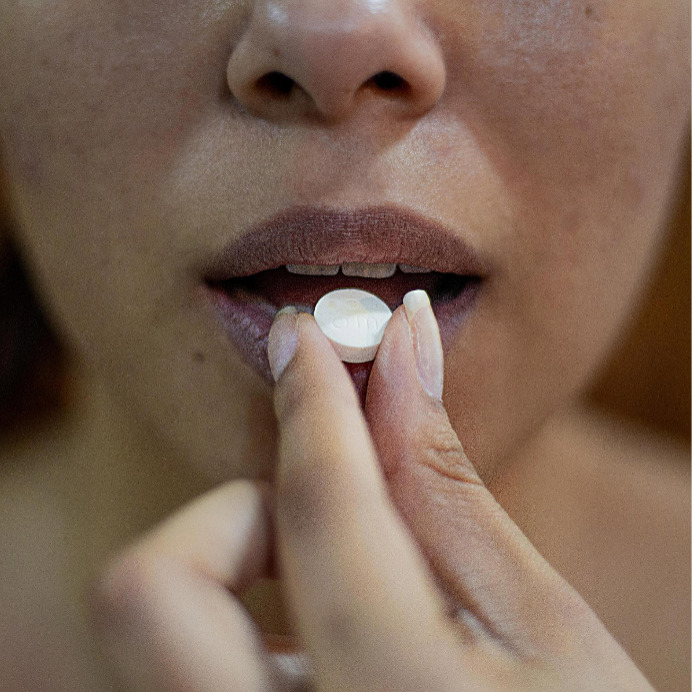
Your Surviving-Tamoxifen Checklist. All the Things You Didn’t Know You Needed, But Do
Nothing can prepare you for the onslaught of side effects the tiny little hormone-blocking drug Tamoxifen can create in your body and your life. At least that’s how I feel…now. When my oncologist first handed me the five-year prescription for the 10-mg daily dose along with a pamphlet listing 40-odd side effects, I thought differently. Then, my oncologist explained how Tamoxifen works and what I may experience—including hot flashes, weight gain and irregular periods—in such an airy, breezy way that took, maybe, all of 45 seconds to share I figured, okay, I’ve got this. This’ll be no big deal. If there was anything to worry about my doctor would warn me. Thousands of women pop this pill every single day without complaint, I’ll be fine.
For the Newly Diagnosed: Part 1
Point of view: You’ve recently been diagnosed with breast cancer, and you’re overwhelmed, confused, scared, and more. You are still having a hard time accepting being diagnosed and don’t know where to start in finding out more medical information about your diagnosis as well as trying to prepare yourself emotionally. While you’ve probably received some type of handout from you doctor, there’s still more information that you need to wrap your head about this change in your life. You’ve also likely searched Google for non-medical information but you are having a hard time finding this information.
Laboratory Blood Tests, Why So Many?
Throughout the course of a medical diagnosis, members of your health care team will order different laboratory blood tests. Many times, these laboratory blood tests will be repeated throughout the diagnosis, treatment, follow-up, and continuing care. Each medical diagnosis and treatment has specific factors that are required to be monitored. When it comes to the results of these tests and what counts are normal or not, it is important to know that “normal” ranges simply reflect average values in a population. It is common for some tests to be slightly outside of the “normal range” (low or high) without consequence and your clinicians can guide you with respect to their relevance.
Three Things to Consider if You’re Thinking About Going Off Tamoxifen
Chances are, if you have breast cancer you’ve heard about Tamoxifen. I remember the first time my oncologist talked to me about the chemo-infused hormonal-therapy drug. It was during my weekly check-up when I was still having daily radiation. He explained that because the cancer cells found in my right breast were 95 per cent estrogen and progesterone receptor positive, my body’s natural hormones could attach to the cancer cells and help them grow. Obviously I didn’t want that, so I said yes to the drug without even hesitating.
Breastfeeding Following a Breast Cancer Diagnosis
Breastfeeding has been linked to a few health benefits such as its ability to reduce the risk of being diagnosed with breast cancer. This may be because of reduced exposure to estrogen as well as the shedding of breast tissue. But what happens when breastfeeding cannot reduce your risk of breast cancer because you have already been diagnosed? While breastfeeding comes with its own challenges, having a newborn while dealing with a breast cancer diagnosis comes with its own unique complications. One of these is knowing whether you can breastfeed your child and how to go about it.
My Temporary Tamoxifen Breakup is Making Me Feel All the Feels
I hope I can write this column without crying. Or at least if I do get emotional, that I won’t need to stop a million times while I wait for the sobbing to ease up so that I can see clearly enough to continue typing. And no, I’m not being dramatic.
CBCN’s Newest Digital Magazine: Complementary Therapies
CBCN produces curated magazines that focus on topics that are relevant to the breast cancer community. These magazines provide patients with an easy-to-access method of getting information on various breast-cancer-related topics. The articles featured in our magazine are pulled from Our Voices blog and are created so that breast cancer patients can access certain themes/topics in one place.
The Impact of COVID-19 on Breast Cancer Patients Part 2: Impact of Your Cancer Treatment and Management on Your Immune System
The risk of a COVID-19 diagnosis for breast cancer patients is still not completely known. Studies have come that show that cancer patients are more at risk of adverse effects if they develop COVID-19. However, a few studies state that compared to other cancer patients, breast cancer patients are at a lower risk of serious illness. The stage of breast cancer also seems to play a role in one’s risk level.
The Impact of COVID-19 on Breast Cancer Patients Part 1: Delayed Surgeries and Treatments
Individuals diagnosed with cancer have been identified as being at a high-risk of getting seriously ill if they get COVID-19. Data from various studies show that the type of cancer, the stage, the person’s age, health, and other factors contribute to how high-risk a patient may be. In addition to this, the type of treatment a person is receiving and how long their last treatment was, can all impact their outcome. At the same time, a few studies have shown that breast cancer patients fare better, compared to patients with other types of cancers.
The flying trapeze artist: Hanging in thin air, waiting for the rest of my life to begin
For Jenn Abbott, finishing treatment for breast cancer is like a flying trapeze. Having received her “NED” (no evidence of disease), she is in mid-air, no longer holding on to the bar that represents the medical team that saved her life, while at the same time, not yet catching the second bar that represents the rest of her life after cancer. She is in limbo, facing post-traumatic stress disorder brought on by her cancer treatment which included five surgeries and a severe adverse reaction to chemotherapy that meant she had to stay in the hospital for two weeks. She feels PTSD after cancer treatment is real.
Ask an expert: Febrile neutropenia explained
Febrile neutropenia, or FN, is a common and potentially serious side effect of chemotherapy treatment.
Cancer-related fatigue Q&A
Because fatigue is a predominant symptom of cancer, CBCN reached out to Georden Jones for advice on managing this symptom. Georden is a doctoral student in clinical psychology at the University of Ottawa. Her thesis focuses on cancer-related fatigue, in particular on the patient's experience with this symptom and how to implement assessment and interventions programs for cancer-related fatigue. Her thesis project is ongoing and is estimated to end by 2019. If you have any questions concerning her work, please do not hesitate to contact her by email: gjone046@uottawa.ca.