By continuing to use our site, you consent to the processing of cookies, user data (location information, type and version of the OS, the type and version of the browser, the type of device and the resolution of its screen, the source of where the user came from, from which site or for what advertisement, language OS and Browser, which pages are opened and to which buttons the user presses, ip-address) for the purpose of site functioning, retargeting and statistical surveys and reviews. If you do not want your data to be processed, please leave the site.
The Voice of People With Breast Cancer
Education
Our Voices Blog
Contributor : CBCN Team
Navigating Emotions, Identities, and Finding Hope
Colleen Packer of Calgary felt a wide range of emotions when she was diagnosed with metastatic lobular breast cancer in 2019: “Shock. Frustration. Fear. Grief. I sobbed. Initially in that first year, it had a really huge impact. Now it has become more routine. Now I feel a lot more in control. It’s a strange mix of feelings to have. It’s both/and. It’s possible to feel happy and sad, angry, grateful, afraid, and confident all at the same time. All those feelings are valid, and you need to provide space for all those feelings because they’re all very much a part of the experience.
Introducing the HAVEN Patient Support Program
Haven is a patient support program by Sentrex that specializes in oncology; this means our all our staff have oncology expertise. In fact, all Haven’s staff have joined Sentrex from hospital cancer centres. Haven offers certain patient support such as insurance reimbursement assistance and pharmacy services.
Paid Breast Cancer Screening: It Can be Worth the Price
Because I’m a born and raised Canadian, I just assumed I would have access to all sorts of free testing and screening when I found the hard, pea-sized lump in my right armpit. Not so much. Here’s how my breast cancer-screening steps went.
Questions & Experts: A General Practitioner in Oncology Answers Your Questions About Post-treatment & Survivorship Care
In today’s post, we provide the questions that were sent in and asked during the live session of our Questions and Experts session held on September 12, 2023. In this session, General Practitioner in Oncology Dr. Anna Wilkinson, FP, GPO answers your questions about post-treatment and survivorship care. In the parentheses, you’ll find the timestamp of where to find the question in the on-demand video.
Stronger Together: Sharing Genes and Breast Cancer Journeys
My name is Cortney Drover, and my identical twin sisters’ name is Connie Claeys. We are 37-year-old females living with Stage IV metastatic breast cancer, and being identical twins, we both carry the BRCA2 gene. Here is our story.
Metastatic Breast Cancer Should be Important to Us All
According to research from the National Cancer Institute, the number of women being diagnosed with metastatic breast cancer is increasing; at the same time, these women are living longer, especially younger women. Living longer with metastatic breast cancer, a stage of breast cancer which is driven in part by out-of-control production of proteins by cancerous cells, means increased needs for services and research.
Stroke, Covid, Cancer: A Caregiver’s Struggle with Breast Cancer
Caregivers are often told, “You need to take care of yourself if you are taking care of others.” It’s so easy to say but not so easy to do. I wrote the above sentence in June 2021 for a future memoir. I had no way of knowing that 15 months later I would be writing about a new challenge. Before I can share my breast cancer story, I need to set the scene.
Free Your Mind: Five Must-know Free Psychotherapy Resources
A breast cancer diagnosis can leave you feeling winded, like you’ve been socked in the stomach and can’t breathe, or even think for that matter. That’s how I felt. I had no emotion, no tears and no anger when I first heard the words “you have breast cancer.” My mind and body simply froze and everything around me, including my mind, went hazy. I attribute this now to shock, which, in my opinion, is a fairly reasonable reaction to receiving such life-changing news. And while the haziness eventually wore off, the surrealness of my new reality remained overwhelming.
How Breast Cancer Transformed Colleen’s Leadership Career
If you found out that you had a life-limiting illness, would you tell your colleagues at work? If you did, would they think you’re less capable of doing your job? That was the dilemma that Colleen Packer faced when she was diagnosed with metastatic breast cancer in 2019.
World Breast Cancer Research Day
In May 2021, The Dr. Susan Love Foundation, one of the top breast cancer research organizations in the United States, announced that every year, August 18th would be known as World Breast Cancer Research Day. The 18th was chosen as a representation of the 1 in 8 women who will be diagnosed with breast cancer during their lifetime. The Foundation also wanted the day to be apart from Breast Cancer Awareness month, which is October, as awareness, patient support, and research need to be highlighted throughout the year. Dr. Susan Love, founder of the Dr. Susan Love Foundation, recently passed away from recurrent leukemia on July 2, 2023. She was a pioneering breast cancer researcher, advocate, surgeon, and fierce critic of the medical field’s historically patriarchal system and paternalistic treatment of women.
Neutropenia and Febrile Neutropenia
Neutropenia is a condition caused by lower-than-normal amounts of neutrophils, a type of white blood cell. Neutrophils fight infection in the body by killing harmful bacteria and other blood-borne pathogens. The most common cause of neutropenia during breast cancer treatment is chemotherapy, though other types of cancer medicine can also cause it. Chemotherapy can cause neutropenia because it kills rapidly dividing cells, such as cancer cells. It can also affect other quickly dividing cells in our bodies, including white blood cells, red blood cells, and platelets. When chemotherapy destroys too many white blood cells, neutropenia occurs.
Ringworm: Tamoxifen’s Secret Side Effect
Trapped beneath my bra, cotton t-shirt and cropped pants, pools of sweat mingled with dust and grime before being absorbed into my clothes and skin. Despite the cold showers I soaped up under twice daily, one before heading out into the wee hours of the morning and another again in the dark of night before crawling under a thin sheet to sleep, the dirty damage was done. A skin fungus had formed. I had ringworm.
Taking the Plunge: Breast Cancer and the Dating Pool
The thought of dating after a breast cancer diagnosis and treatment might make you nervous or excited. It may also reawaken or increase emotional responses you had at diagnosis or during treatment. If you have anxiety or depression, these responses can cause you to focus on or magnify negative thoughts about your prospects for dating. If you want to date but feel reluctant to start, you might be having difficulty imagining yourself meeting new people and having fun.
FinNav Five: Government Programs
The negative financial impacts after a breast cancer diagnosis can be strenuous, especially for those already in a precarious financial situation prior to being diagnosed. Already having to deal with the overwhelming feeling of being diagnosed with breast cancer, patients should be able to focus on their health and not have the added stress of dealing with their financial situation. That is why we created FinancialNavigator, an online database of various financial assistance programs across Canada.
Highlights from ASCO 2023
The 2023 American Society of Clinical Oncology (ASCO) annual meeting was held from June 2 to 6. CBCN was pleased to be able to attend and participate in the many interesting and groundbreaking research that was shared at ASCO this year. Below, we present a few highlights and takeaways from this year’s conference.
Show Me the Money. Five Ways You Can Receive Financial Support
When I was diagnosed with breast cancer, I had no idea how hard it would be. Not the surgery, I’ve had major surgery before, so I wasn’t afraid of being put under anesthetic and being operated on. Mentally, I was focused on one sole factor, survival, so my head space at the time was very clear and didn’t allow for any other emotions or thoughts. Reality, fear, anxiety, hope…that all came later.
Addressing the Healthcare Needs of Indigenous Populations
June 21, 2023 is National Indigenous Peoples Day. This is a day for all Canadians to recognize and celebrate the unique heritage, diverse cultures and contributions of First Nations, Inuit, and Métis peoples. This is also a day that should call to attention the various issues that Indigenous peoples continue to face, including racism, colonialism, and disparate health outcomes from much of the rest of Canada. Broad determinates of health like geography, accessibility and availability of services, and cultural differences contribute to the challenges faced by Indigenous peoples.
Do You Feel Invisible?
A few years ago, a friend shared a story about the first trimester of her pregnancy. She was thrilled to be pregnant, but at the time, kept her pregnancy under wraps as she hadn’t passed the three-month safety zone. She was also sick as a dog, overwhelmed with intense nausea and fatigue, that heightened during her twice-daily, 25-minute subway commute to and from work. Despite looking green-ish, sweaty, unstable on her feet and gripping whatever pole or hand railing was available, not once in 90 days did anyone sitting on the subway offer my friend their seat. She’d felt invisible.
FinNav Five: Funds and Grants
Depending on your situation, your financial needs can come in different forms, from needing money to pay for rent, to needing help with paying for treatments, to requiring help with parking costs when you go for cancer treatments. To highlight the various types of programs listed in FinancialNavigator, we have put together this blogpost series. All the highlighted programs below are available to individuals in all provinces and territories, unless otherwise noted. This is not an exhaustive list all of programs in these categories but is meant to highlight the types of financial help that can be found in our FinancialNavigator database. Visit FinancialNavigator for all available financial assistance programs.
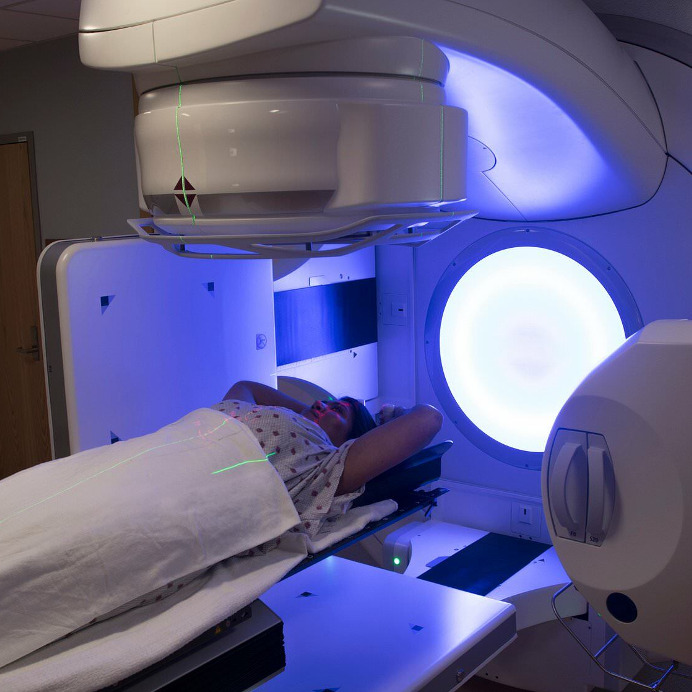
Reason #5 Cancer Still Sucks: Radiation Therapy is Hit or Miss
The fifth reason that cancer still sucks is that although radiation therapy can be an effective cancer treatment, it may fail to kill some of the tumor cells in its path, or it may miss some tumor cells completely. In addition, while “palliative” radiotherapy can dramatically improve symptoms in some individuals with incurable cancers, it may have minimal impact or provide only very brief relief to others.