By continuing to use our site, you consent to the processing of cookies, user data (location information, type and version of the OS, the type and version of the browser, the type of device and the resolution of its screen, the source of where the user came from, from which site or for what advertisement, language OS and Browser, which pages are opened and to which buttons the user presses, ip-address) for the purpose of site functioning, retargeting and statistical surveys and reviews. If you do not want your data to be processed, please leave the site.
The Voice of People With Breast Cancer
Education
Our Voices Blog
Tag : diagnosis
From “Am I Going to Die?” to Living Life Over Cancer
“Am I going to die?”
That was the first question I asked when I was told I had breast cancer.
Many people face this difficult question after a diagnosis, which can bring fear, uncertainty, and overwhelm. It can also feel, at times, as if the future you had imagined is being taken from you.
What We Don’t Know (and it’s a lot), Should Know, About Canada’s Breast Cancer Screening Guidelines
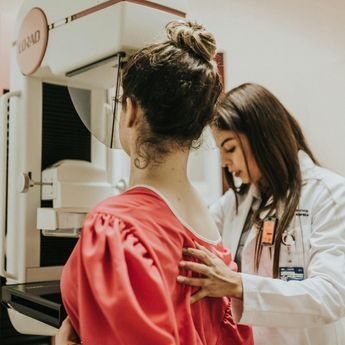
How old were you when you first learned you were eligible for a mammogram? If you’re like me, that information only became clear after you found a lump of your own. And at that point, the rules and guidelines about when women can and can’t access breast cancer screening don’t feel relevant anymore—it’s too late. Except that it shouldn’t be.
Before You Ask AI About Your Health, Read This
Over the past year, something important has shifted in how people look for health information. More patients are turning to artificial intelligence (AI) tools like ChatGPT, not to replace their doctors, but to fill the long stretches of uncertainty between appointments.
The Messy, Honest Truth About Diagnosis, Recovery and the Emotions No One Talks About
I’m an open book about breast cancer. I’ve chosen to be vocal because I want to wipe out stigma, shine light on little-talked about topics and help other women feel less alone. When I was first diagnosed with breast cancer, it didn’t cross my mind that one day I’d want to share all the details about my personal experiences with cancer by writing a monthly column, but life is weird and here I am. And I’m grateful. Especially when I receive a direct message on my Instagram from a woman I don’t know, who is dealing with her own breast cancer diagnosis and looking for support.
Charting a Different Course
Jeanne lost her mother when she was 25, and her aunt also had breast cancer. When Jeanne was diagnosed with triple-negative breast cancer (TNBC), her children were still very young. In her blog, www.triplenegatif.blogspot.com, Jeanne returns to the multiple aspects of the breast: that of the woman, the mother, the sick person, then the reconstructed breast. Heredity and lineage, but also faith, are questioned in a lyrical, almost poetic and soul-searching way.
Busting Breast Cancer Myths: You Can’t Get Breast Cancer Without a Family History
Having a family history of breast cancer could mean two different things. About 5% to 10% of breast cancer cases are passed down from parent to child. Sometimes, several people in a family may have breast or other types of cancer. But even when no inherited or familial connection is found, breast cancer can still happen unexpectedly.
Dancing Through Diagnosis, part 2
There was a total of three oncologists from different areas of care that I would meet along the way. Then there is my plastic surgeon! The beginnings of a joke. Three oncologists and a plastic surgeon go into a bar... If you have a good joke for this scenario, I would love to hear it. But this is the thought that keeps popping into my head every time I am told about my surgical team.
Dancing Through Diagnosis, part 1
As my towel brushed past the bottom of my right breast, I couldn’t help noticing that something didn’t feel right. Broken glass? It felt like broken glass. Is that possible? Could I have broken my boob? Can you break a boob? My mind began to swirl toward real questions then to ones that were clearly insane and made no sense... and yet, I asked them out loud... to myself... in the mirror.
Embracing a New Normal Through Strength and Hope
My cancer journey began when I noticed my right breast leaking. I honestly chalked it up to a hormone imbalance and thought nothing of it until six months later, when the leaking had not subsided, and my breast had become very itchy. During this time, I had also noticed how tired and fatigued I was every day. I found myself napping a lot and needing that nap to just make it through the day. I decided that I better make a doctor’s appointment to see what was going on with my body.
Making Powerful Healthcare Decisions - Claim Your Voice
Having a solid strategy for gathering trusted and dependable information is critical for making informed treatment decisions when it comes to your health. It is also important to be able to communicate assertively with healthcare practitioners as an equal partner in shared decision-making.
How and When to Drop the Big-C News
I don’t know what it was like for you but for me, saying “I have breast cancer” out loud felt fake, like I was lying. Every time the words came out of my mouth I wanted to hide. Rationally, I knew my diagnosis was real, but the horrible emotions that preceded and followed each proclamation filled me with shame. And the voice inside my head was relentless. It just kept goading me on.
The Must-Know Info About Early-Stage Breast Cancer
As I tried to process my diagnosis and what it meant for me, along with the future I’d envisioned for myself, I went into research mode. It’s my comfort zone. I’m curious by nature and profession (being a writer and all), and having information, knowing everything that I need to know, makes me feel in control. So, I dug deep, Googled like a crazed person, and asked my doctors hundreds of questions while I tried as best as I could to prepare myself for the unknown that was to come. Here’s what I learned about being diagnosed with early-stage breast cancer.
Younger Women and Breast Cancer Care Equity
The spending justifications for girl math are funny. But they just aren’t real. And oddly, this type of rationalization reminds me of how many doctors dismiss younger women when they believe that they have breast cancer. I know this because it happened to me. This is how I see girl math being applied to breast cancer.
Navigating Life's Tough Challenges: Building Resilience in the Face of Adversity
When I received the news that I had breast cancer, my world seemed to crumble before my eyes. Overwhelmed, vulnerable, and defenseless, I faced a daunting journey ahead. As a seasoned business owner, I had encountered my fair share of adversity, but nothing could prepare me for this level of fear. For the first time, I found myself fearing the unknown, dreading the loss of everything: my health, my quality of life, my business, and all my assets. How could I possibly endure this?
Navigating Emotions, Identities, and Finding Hope
Colleen Packer of Calgary felt a wide range of emotions when she was diagnosed with metastatic lobular breast cancer in 2019: “Shock. Frustration. Fear. Grief. I sobbed. Initially in that first year, it had a really huge impact. Now it has become more routine. Now I feel a lot more in control. It’s a strange mix of feelings to have. It’s both/and. It’s possible to feel happy and sad, angry, grateful, afraid, and confident all at the same time. All those feelings are valid, and you need to provide space for all those feelings because they’re all very much a part of the experience.
How Breast Cancer Transformed Colleen’s Leadership Career
If you found out that you had a life-limiting illness, would you tell your colleagues at work? If you did, would they think you’re less capable of doing your job? That was the dilemma that Colleen Packer faced when she was diagnosed with metastatic breast cancer in 2019.
The Cancer Time Warp
It’s safe to say that most of us believe, kind of like the-sky-is-blue believe, that the past, present, and future are the logical chronology of time. Even mathematical equations, which I am terrible at, define time as the measure of the duration that exists between each sequence of these events. So how come when it comes to breast cancer, time is so fucked up? It would be so much more manageable if we, individuals diagnosed with cancer, could just live in the present.
What You Believe Will Be
Don’t curse me if this column sounds crazy. Or do. It’s up to you. But what I’m sharing in this column is true for me and it has changed my life for the good. Trust me, as a single woman who lives alone with her two cats, is constantly hustling to secure editorial work and hasn’t had a single decent “like” on Hinge in well over a year, I’m always looking for the positive. This is my honest-to-goodness M.O.
Breast Self-exams. Why you still need to do them even with a cancer diagnosis
Feel it on the first. Know your lemons. Check your boobies. Get in touch with them apples. I never noticed these catch phrases written on social media to inspire women to do monthly breast self-exams until after I was diagnosed. Well after too, like, when I was recovering from having had breast cancer surgery and treatment. Ironic, isn’t it? More ironic is the fact that I never really did regular breast self-examinations on my boobs and when I did, they were always half-hearted, like an afterthought.
Reason #4 That Cancer Still Sucks: Surgery Can’t Prevent Recurrence
In this blog series, we present excerpts from Dr. David Stewart’s book A Short Primer on Why Cancer Still Sucks. The fourth reason that cancer still sucks is that it can recur in some patients even if it appears to have been removed completely by surgery. Surgery is not even an option for many patients.